Surgical Scars
A surgical scar is a thick, raised scar that is an abnormal response to surgical wound healing. Surgical scars do not usually blend with the tone and texture of the surrounding skin. Depending on the shape, size, and location, they can be noticeable—even wound healing results in less visible scars.
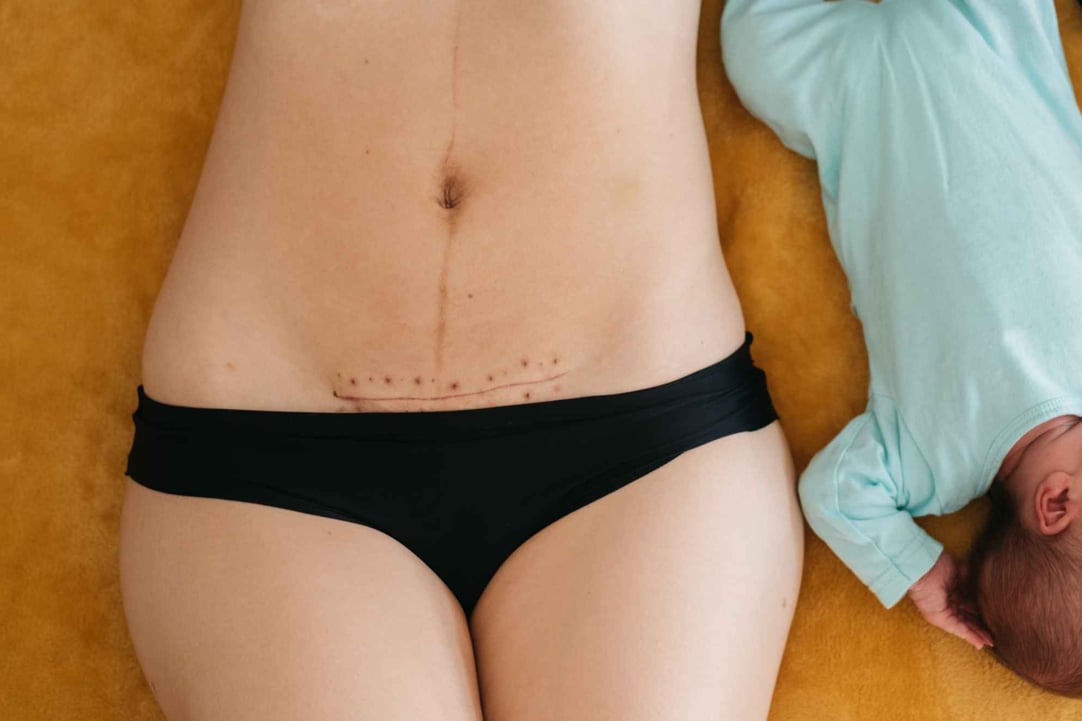
What is Surgical Scars
Scarring is a natural part of wound healing after the surgical excision or incision of tissue. Surgical scars are undesirable outgrowths of tissue that develop in response to wound healing. Surgical scars grow in all sizes and shapes. Most surgical scars fade over time but never disappear completely—some are awkwardly prominent, while others are hardly visible.
Characteristics of a cosmetically acceptable surgical scar are:
It should be a hardly noticeable fine line.
It should be parallel to skin creases and folds.
It should have similar color and shape as the surrounding skin.
There should be no disfigurement of the adjacent structures.
It should be at the level of the skin.
It should be well-settled on the tissue.
A surgical scar that restricts the mobility or function of tissue is considered unfavorable. Undesirable surgical scars may be wide, pigmented, raised, pitted, or transverse through natural creases, folds, and junctions.
Age is an important factor contributing to surgical scar formation. Surgical scars are observed with lesser frequency in the elderly. It contrasts surgicall scars in children, among whom they are common because of increased cellular activity, prolonged scar maturation, rapid physical growth, and increased skin elasticity. Other factors include poor wound healing, ethnic background, and genetics.
Common Types of Surgical Scars
Scars may be formed for many reasons, including infections, surgery, injuries, or tissue inflammation. Several types of surgical scars include keloid, hypertrophic, and atrophic scars. Each type of scar has unique characteristics and may require different treatment approaches for optimal healing and cosmetic outcomes.
Hypertrophic Scars
A hypertrophic scar has its surface elevated compared to the surrounding normal skin. Hypertrophic scars commonly develop in areas where the skin is taut, such as your back, chest, upper arm, shoulders, elbows and other joints. However, hypertrophic scars can develop anywhere on your skin where you have a skin injury or wound.
Like keloid scars, hypertrophic scars result from excess collagen production at the wound's site. However, unlike keloid scars, hypertrophic scars do not exceed the wound margin.
Hypertrophic scars are often red and grow from 3 to 6 months. Most hypertrophic scars begin to lose the redness and reduce in size around 6 months, and continues for 2 years until the elevated surface flattens.
Keloid Scars
Keloids are frequently observed in wounds experiencing high stress. Predisposition to keloids is known to be passed down from particular ethnic backgrounds, as they are more commonly found in Africans and Asians—populations of African descent experience keloid formation as high as 4.5 to 16 percent.
The feature discerning keloids from hypertrophic scars is their continued growth during the later phase of the collagen remodeling process between 6 and 18 months. A keloid scar grows beyond the wound margin, turns red to brown, behaves like a benign skin tumor, and may also affect mobility.
Atrophic Scars
Atrophic scars are also known as pitted scars or ice-pick. They are formed when healing takes place below the surface of the skin. They are sunken scars, often resulting from chickenpox and acne, and sometimes due to trauma, genetic disorders, or injuries that damage or remove skin tissue, such as cuts, burns, or surgical incisions, for example, mole removal surgery.
Atrophic scars can leave a person feeling uncomfortable or embarrassed about their physical appearance and may affect their social interactions and overall quality of life.
What Causes Surgical Scars
Surgical scars commonly occur after surgeries, and several factors can influence their appearance. Causes of surgical scars include the type of surgery performed, the surgical technique used, the patient's age and skin type, and their overall health and ability to heal. Knowing the right cause of surgical scars is imperative to planning the right treatment strategy.
Incision size and depth
The size and depth of the surgical incision can affect the resulting scar's appearance and healing process.
Tension on the wound
Excessive tension on the wound during the healing process may lead to more noticeable or widened scars.
Genetics
Genetic factors can influence an individual's predisposition to developing certain types of scars, such as keloids or hypertrophic scars.
Infection
Infections occurring at the surgical site can disrupt the healing process and increase the likelihood of scar formation. Infections occurring at the surgical site can disrupt the healing process and increase the likelihood of scar formation.
Procedures That Remedy Surgical Scars
Surgical scar appearance is often a major concern among patients, with many seeking advice from their surgeons regarding scar management. Many over-the-counter products claim to decrease surgical scar formation and improve wound healing. These products attempt to create an ideal environment for wound healing with varying level of success rate. However, no treatment modality can permanently remove the surgical scars. A few most effective treatment regimes for surgical scars are discussed below:
Topical treatments
Silicone ointment, corticosteroid cream, silicone gel sheets, and skin-lightening creams with hydroquinone are all potential treatments for scars. However, the effectiveness of each treatment can vary depending on the type and severity of the scar, the individual patient's skin type, and other factors. Your healthcare provider can help you determine the best treatment for your needs and circumstances.
Steroid injections
Corticosteroid injection is a commonly used treatment for surgical scars. Corticosteroids reduce inflammation and suppress the immune response, which can help reduce scar tissue formation. The injections are typically administered directly into the scar tissue. They may need to be repeated several times over weeks or months to achieve optimal results.
Surgical revision
Surgical revision of incisional scars does not erase a scar but helps to make it less noticeable and more acceptable. A fundamental principle of surgical scar revision is to minimize the incorporation and disfigurement of the surrounding normal tissue as much as possible.
The various surgical techniques for revising the scar are:
Fusiform elliptical excision
Z-plasty
Half Z-plasty
Four flap Z-plasty
Planimetric Z-plasty
S-plasty
W-plasty
Geometric Broken Line Closure (GBLC)
V-Y and Y-V advancement
Flaps and grafts
Frequently Asked Questions
How long does it take for a surgical scar to heal?
While the initial healing of a surgical incision can take around 2 weeks, it can take several months for the scar to mature and become pale and flat fully. During this time, the scar may go through various stages of healing, including inflammation, collagen production, and remodeling, which can affect the appearance and texture of the scar. Proper wound care can help promote optimal healing and minimize scarring, such as:
Keeping the area clean
Keeping surgical site moisturized
Protecting it from the sun
Avoiding activities that could stress the healing tissue
Can surgical scars be prevented?
Avoiding stress on your incision is important in promoting optimal healing and minimizing scarring. Activities that stress the wound, for example, bending, stretching, and twisting should be avoided until your healthcare provider has given you the go-ahead to resume normal activities. Additionally, protecting your incision from exposure to sunlight can help to prevent or minimize visible surgical scars. UV radiation can damage the healing tissue and cause hyperpigmentation, making scars more noticeable. Wearing loose, comfortable clothing that covers the incision site and applying sunscreen to the area can help protect your surgical site and promote optimal wound healing.
What can I do to minimize the appearance of my surgical scar?
Following these steps can help reduce the appearance of your surgical scars:
Use topical creams
Practice proper wound care
Use scar therapy products
Eat a healthy balanced diet with plenty of protein
Let your doctor know if you're prone to raised scars (also called keloid scars)
Massage the scar tissue
Protect your surgical site from sun
Consider laser therapy or scar revision surgery
Are there any risks or complications associated with surgical scar revision?
As with any surgical procedure, there is a risk of infection, bleeding, and adverse reactions to anesthesia. Other potential complications may include poor wound healing, scarring, changes in skin sensation, and asymmetry.
It's important to discuss the risks and benefits of scar revision surgery and your individualized case and potential outcomes with your surgeon before the scar revision surgery. Having realistic expectations and being fully informed before deciding whether scar revision surgery is right for you is important.